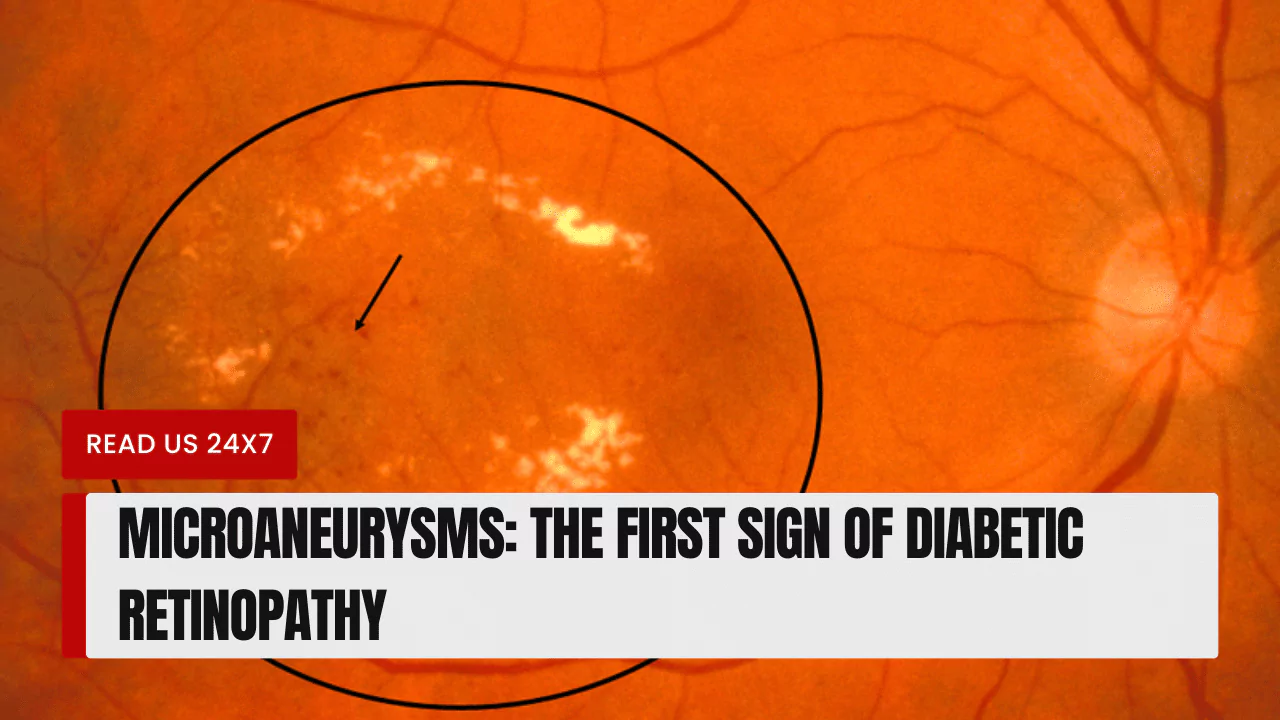
Microaneurysms are tiny, ballooning blood vessels in the retina, the light-sensitive tissue at the back of the eye. They are the earliest visible sign of diabetic retinopathy (DR), a serious eye complication of diabetes.
DR is a leading cause of blindness in adults. It develops when high blood sugar levels damage the blood vessels in the retina. Over time, this damage can lead to a variety of eye problems, including microaneurysms.
Understanding Diabetic Retinopathy
What is Diabetic Retinopathy?
DR is a progressive disease that affects the blood vessels in the retina. There are two main types of DR: nonproliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR).
- NPDR is the early stage of DR. In NPDR, the blood vessels in the retina leak blood and fluid. This can cause microaneurysms, as well as other changes in the retina, such as hard exudates (yellow deposits) and soft exudates (cotton wool spots).
- PDR is the more advanced stage of DR. In PDR, new, abnormal blood vessels grow on the surface of the retina. These blood vessels are weak and can leak blood, which can lead to vision loss.
Causes and Risk Factors
The main cause of DR is high blood sugar levels. Other risk factors for DR include:
- Duration of diabetes: The longer you have diabetes, the higher your risk of developing DR.
- Type of diabetes: Type 1 diabetes is associated with a higher risk of DR than type 2 diabetes.
- High blood pressure
- High cholesterol
- Pregnancy
The Role of Microaneurysms in Diabetic Retinopathy
What are Microaneurysms?
Microaneurysms are tiny, ballooning blood vessels in the retina. They are caused by damage to the blood vessel walls. Microaneurysms are usually red in color and appear as small dots on the retina.
Why Do They Occur in DR?
High blood sugar levels can damage the blood vessel walls in the retina. This damage can lead to the formation of microaneurysms.
Relationship to Other Signs of DR
Microaneurysms are often the first visible sign of DR. However, they can also occur in other eye conditions, such as retinal vein occlusion and radiation retinopathy.
Diagnosis and Treatment
How is DR Diagnosed?
DR is diagnosed during a comprehensive eye exam. This exam includes a dilated eye exam, in which the doctor uses eye drops to widen the pupils so they can get a better view of the retina.
Treatment options for DR
There is no cure for DR, but there are treatments that can help slow the progression of the disease and prevent vision loss. Treatment options for DR include:
- Blood sugar control: Good blood sugar control is essential for preventing and managing DR.
- Laser photocoagulation: This procedure uses a laser to seal off leaking blood vessels.
- Anti-VEGF injections: These injections are used to block the growth of new, abnormal blood vessels.
- Surgery: In some cases, surgery may be necessary to remove scar tissue or abnormal blood vessels from the retina.
Long-Term Vision Implications
Impact of Microaneurysms on Vision
Microaneurysms can cause vision problems in several ways. They can leak blood and fluid into the retina, which can blur vision. They can also block the flow of blood to the retina, which can damage the light-sensitive cells in the retina and lead to vision loss.
Prognosis and Complications
The prognosis for DR depends on the severity of the disease and the effectiveness of treatment. With early diagnosis and treatment, most people with DR can maintain good vision. However, if DR is left untreated, it can lead to serious complications, such as blindness.
Tips for Managing Diabetes to Reduce Risk of DR
There are several things you can do to manage your diabetes and reduce your risk of developing DR:
- Keep your blood sugar levels under control.
- Get regular eye exams.
- Maintain a healthy weight.
- Eat a healthy diet.
- Exercise regularly.
- Avoid smoking.
Conclusion
Microaneurysms are the first visible sign of DR, a serious eye complication of diabetes. Early diagnosis and treatment of DR can help prevent vision loss. If you have diabetes, it is important to get regular eye exams to check for signs of DR.